Dental Implants have high rates of long term survival, defined as more than 10 years when supporting various dental prostheses. However, the success of dental implants is not as high as their survival as functional implants and the restorations may be subject to mechanical and biological complications. Biologic complications associated with dental implants are mostly inflammatory conditions of the soft tissues and surrounding bone.
These are biofilm-induced inflammatory lesions around dental implants. A survey of American, Australian, and European periodontists revealed no consensus in understanding the etiology of peri-implant diseases nor their diagnosis and management. The combined workshop aimed to establish clinical guidelines for diagnosis, classification, and treatment of peri-implantitis, and peri-implant mucositis.
The objective of this review is to identify case definitions and clinical criteria of peri‐implant healthy tissues, peri‐implant mucositis, and peri‐implantitis. The case definitions were constructed based on a review of the evidence applicable for diagnostic considerations.
The diagnostic definition of peri‐implant health is based on the following criteria:
1) absence of peri‐implant signs of soft tissue inflammation (redness, swelling, profuse bleeding on probing)
2) the absence of further additional bone loss following initial healing.
The diagnostic definition of peri‐implant mucositis is based on the following criteria:
1) the presence of peri‐implant signs of inflammation (redness, swelling, line or drop of bleeding within 30 seconds following probing)
2) no additional bone loss following initial healing.
The clinical definition of peri‐implantitis is based on the following criteria:
1) the presence of peri‐implant signs of inflammation
2) radiographic evidence of bone loss following initial healing
3) increasing probing depth as compared to probing depth values collected after placement of the prosthetic reconstruction. In the absence of previous radiographs, a radiographic bone level more or equal to 3 mm in combination with BOP and probing depths more or equal to 6 mm is indicative of peri‐implantitis.
IMPLICATIONS FOR PATIENT CARE
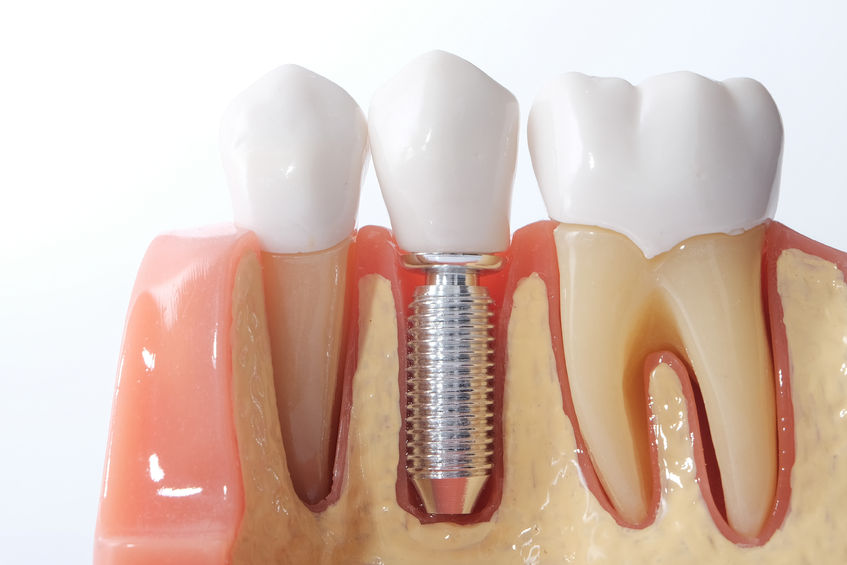
IMPLANT
1. Clinical evaluation of the soft tissue conditions around implants should include registration of oral hygiene in general, with a specific focus on the presence of biofilm on implants and their restorations.
2. Dental implants should be visually evaluated and probed routinely and periodically (at least once per year) as part of comprehensive oral exams, similar to natural teeth.
3. Pocket probing on dental implants should be conducted with a light force (approximately 0.25 N); peri‐implant pocket depths should in general be less or equal to 5 mm.
4. Bleeding on probing should not occur at implant sites defined as being healthy. Bleeding on probing should be assessed carefully using light forces (0.25 N) to avoid possible effects of trauma caused by the process. It is difficult to differentiate between biofilm‐induced peri‐implant inflammation and mechanically‐induced trauma; bleeding “dots” should be interpreted carefully as this may represent bleeding due to tissue trauma and not bleeding associated with tissue inflammation.
5. Intra‐oral radiographic evaluation of changes in bone levels around implants (preferably using a standardized film holder) is necessary to discriminate between health and disease states. A prerequisite for the radiographic evaluation should be an image taken at baseline (supra‐structure in place) that clearly allows for identification of an implant reference point and distinct visualization of implant threads, for future reference as well as assessment of mesial and distal bone levels in relation to such reference points.
6. Absence of bone loss beyond bone level changes resulting from initial bone remodeling. Alveolar bone remodeling following the first year in function may be dependent on the type and position of the implant, but change (loss) of alveolar bone starting after the implant was placed in function should not exceed 2 mm. Changes more or equal to 2 mm at any time point during or after the first year should be considered as pathologic.
What Clinical and Radiographic Findings and What Clinical Examination Steps are Necessary to Detect the Presence of Peri-Implant diseases? Peri-Implant Mucositis

1. Visually, local swelling, redness, and shininess of the soft tissue surface are classical signs of clinical inflammation. A common symptom reported by patients is soreness.
2. A local dot of bleeding resulting from probing may be the result of a traumatic (probing) injury that should not be considered, in the absence of other inflammatory changes, a definitive criterion to characterize a peri‐implant soft tissue lesion.
3. Any bleeding on probing that is combined with visual inflammatory changes of the tissues at the site of Probing.
4. Clear evidence of bleeding such as a line of bleeding or drop bleeding should be used as an indication of an inflammatory peri‐implant soft tissue lesion.
5. Suppuration upon clinical examination (e.g., application of light pressure to the tissues or following probing).
6. Intra‐oral radiographic evaluation of bone levels around implants should always be included in the presence of clinical signs of inflammation. In addition, a pre‐requisite for the evaluation is that a radiograph is taken at baseline (supra‐structure in place) and used for future assessment of mesial and distal bone levels in relation to defined references.
Accounting for the remodeling process of alveolar bone during the first year after installation, the change in bone level since the placement of the prosthetic supra‐structure should not be more or equal to 2.0 mm. Presence of bone loss beyond crestal bone level changes resulting from the initial remodeling process of alveolar bone after implant installation suggests either progressive peri‐implant infection or other local factors such as excess cement and looseness/fracture of implant components.
PERI-IMPLANTITIS

1. The visual inspection with assessment of the presence of classical signs and symptoms of inflammation, i.e. redness, swelling, pain, and bleeding on probing (characteristics of the latter, described for peri‐implant mucositis, also apply to the diagnosis of peri‐implantitis).
2. The differential diagnosis between peri‐implant mucositis and peri‐implantitis is based on evidence that alveolar bone loss following initial healing and bone remodeling has occurred and requires a radiographic evaluation of the bone level around dental implants over time. This is in addition to the presence of inflammatory changes and bleeding on probing on a given site.
3. Presence of bone loss beyond crestal bone level changes resulting from the initial remodeling in conjunction with BOP after the implant has been placed in function should be considered as a marker for peri‐implantitis.
4. Radiographs should be taken based on the clinical judgment after findings. Standardized radiographs should be taken and compared to reference radiographs when the implant(s) was placed in function.
Some of Our Long-Term
Results

Our mission
It is the mission of this office to provide our patients with the highest level of excellence in oral health care.
Our team is thoroughly committed to excellence for our patients; you’ll be treated with dignity and respect in a trusting, open, honest environment and the confidential nature of your personal information will be recognized and respected.
Decisions are made with our patients on the basis of consensus, valuing diversity of opinion, in an environment that fosters mutual respect.