A committee representing both the American Academy of Periodontology (AAP) and the European Federation of Periodontology (EFP) met in November 2017 with the charge of updating the 1999 classification of periodontal disease and conditions. The Proceedings of the World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions consists of 19 review papers and four consensus reports.
This post provides a simple summary of the new classification of periodontal disease and peri-implant disease, as well as discusses the staging and progression of periodontitis. This information can be used to explain treatment needs to both patients and insurance companies.
For more detailed information regarding changes to disease classification, it is recommended that the full proceedings of the World Workshop of the AAP and EFP be consulted.
According to the new classification scheme, periodontal disease and conditions can be broken down into three major categories, each with subcategories.
Periodontal disease and conditions can be broken down into three major
categories:
1. Periodontal health and gingival diseases
a. Periodontal and gingival health
b. Gingivitis caused by biofilm (bacteria)
c. Gingivitis not caused by biofilm
2. Periodontitis
a. Necrotizing diseases
b. Periodontitis as a manifestation of systemic disease
c. Periodontitis (more detailed explanation below)
3. Other conditions affecting the periodontium
a. Systemic diseases affecting the periodontium
b. Periodontal abscess or periodontal/endodontic lesions
c. Mucogingival deformities and conditions
d. Traumatic occlusal forces
e. Tooth- and prosthesis-related factors
According to the new classification, when describing periodontitis, we now must clarify the stage and extent, and grade the progression with anticipated treatment response. The staging of periodontitis is based on both severity and complexity of management.
Grading of periodontitis (assessing rate of progression and anticipated response to treatment):
1. Grade A (slow progression)
No BL or CAL over five years, no smoking, no diabetes, heavy biofilm but no
Destruction
2. Grade B (moderate progression)
Less than 2 mm BL or CAL over five years, half pack or less per day smoking,
HbA1c less than 7%, biofilm commensurate with destruction
3. Grade C (rapid progression)
Greater than 2 mm of BL or CAL over five years, half pack or more per day
smoking, HbA1c 7% or higher, destruction exceeds amount of biofilm
Extent and distribution of
periodontitis:
1. Localized— BL is around less than 30% of teeth in mouth
2. Generalized— BL is around more than 30% of teeth in mouth
3. Molar-incisor— BL is found around molar (usually first) and anterior incisors
Staging of periodontitis:
- Stage I (initial)
1–2 mm clinical attachment loss (CAL), less than 15% bone loss (BL) around root, no tooth loss due to periodontal disease, probing depth (PD) 4 mm or less, mostly horizontal BL (figure 1)

2. Stage II (moderate)
3–4 mm CAL, 15%–33% BL, tooth loss, PD 5 mm or less, mostly horizontal BL
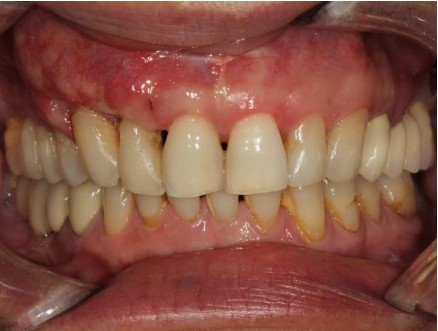
3. Stage III (severe with potential for additional tooth loss)
5 mm or more CAL, BL beyond 33%, tooth loss of four teeth or less, with complex issues such as PD 6 mm or more, vertical BL 3 mm or more, Class II–III bifurcations, and/or moderate ridge defects
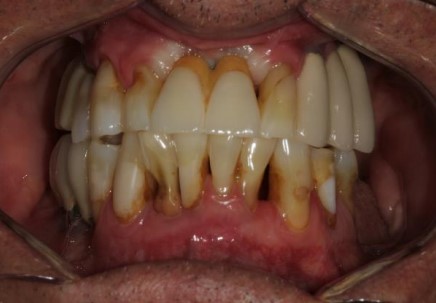
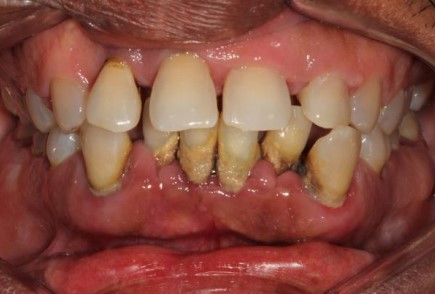
4. Stage IV (severe with potential for loss of dentition)
Encompasses all of Stage III with additional features that will require the need for complex rehabilitation due to masticatory dysfunction, secondary occlusal trauma, severe ridge defects, bite collapse, pathologic migration of teeth, less than 20 remaining teeth (10 opposing pairs)
Our mission
It is the mission of this office to provide our patients with the highest level of excellence in oral health care.
Our team is thoroughly committed to excellence for our patients; you’ll be treated with dignity and respect in a trusting, open, honest environment and the confidential nature of your personal information will be recognized and respected.
Decisions are made with our patients on the basis of consensus, valuing diversity of opinion, in an environment that fosters mutual respect.